

May 2012
IN THIS ISSUE:
![]()
- Clinical Center Nutrition Department feeds young minds at science festival
- Researchers find method to improve transplant cell delivery
- Longtime Clinical Center advocate Susan Butler honored
- Department of Transfusion Medicine staff member mourned
- Mannes named Department of Perioperative Medicine chief
- Practice makes perfect—Staff tests emergency preparedness skills
- Patient tracking and locating system wins HHSinnovates award
- Patient safety interventions at CC reduce risk, improve care
- DLM staff saluted during lab week
- Medical Record Department celebrates health information professionals week
- CC hosts annual pharmacology meeting
- Office of Workforce Management and Development quick tip: staying motivated
- Clinical Center news briefs
- Upcoming Lectures
- New Clinical Research Protocols
Print this Issue ![]() (394 KB)
(394 KB)
ABOUT CC NEWS:
![]()
Published monthly for CC employees by the Office of Communications, Patient Recruitment, and Public Liaison. News, article ideas, calendar events, letters, and photographs are welcome. Submissions may be edited.
Clinical Center News
National Institutes of Health
Building 10, 10 Center Drive
Room 12C440,
Bethesda, MD 20892-1504
Tel: 301-496-6787
Fax: 301-402-1982
Lipsett Amphitheater, 12 noon
Lectures will be videocast.
May 2
Contemporary Clinical Medicine: Great Teachers
Colon Cancer Screening: Evolution Toward Eradication
David A. Johnson, MD
Professor of Medicine and Chief of Gastroenterology, Eastern Virginia Medical School
Case Presenter: Marion Danis, MD, Chief, Bioethics Consultation Service and Head, Section on Ethics and Health Policy, Department of Bioethics, CC
May 9
Reframing Informed Consent: Understanding How Research Participants Make Decisions
Gwenyth R. Wallen, RN, PhD
Chief, Nursing Research and Translational Science, Nursing and Patient Care
Services, CC
Christine Grady, MSN, PhD
Chief, Department of Bioethics, CC
Connie Ulrich, RN, PhD
Associate Professor, School of Nursing, and Department of Medical Ethics and Health Policy, School of Medicine, University of Pennsylvania
**Lecture will be held in Masur Auditorium
May 16
Development of Therapeutic Interventions for Niemann-Pick Disease, Type C1
Forbes D. Porter, MD, PhD
Clinical Director and Acting Head, Program on Developmental Endocrinology and Genetics, NICHD
From Metabolism to Immunity: The Story of Type I Glycogen Storage Disease
Janice Y. Chou, PhD
Chief, Section on Cellular Differentiation, Program on Developmental Endocrinology and Genetics, NICHD
May 23
Idiopathic CD4 Lymphopenia: Still More Questions Than Answers
Irini Sereti, MD
Tenure Track Investigator and Head, HIV Pathogenesis Unit, Laboratory of Immunoregulation, NIAID
The Genetics of Melanoma: Searching for New Therapeutic Targets
Yardena Samuels, PhD
Tenure Track Investigator and Head, Molecular Cancer Genetics Section, Cancer Genetics Branch, NHGRI
May 30
Magnetic Resonance Imaging in Acute Traumatic Brain Injury: Identification of Novel Biomarkers and Implications for Therapy
Ramon Diaz-Arrista, MD, PhD
Director of Clinical Research, Center for Neuroscience and Regenerative Medicine, and Professor of Neurology, Uniformed Services University of the Health Sciences
The Genetics of Melanoma: Searching for New Therapeutic Targets
Yardena Samuels, PhD
Tenure Track Investigator and Head, Molecular Cancer Genetics Section, Cancer Genetics Branch, NHGRI
Lawrence L. Latour, PhD
Staff Scientist, Section on Stroke Diagnostics and Therapeutics, Division of Intramural Research, NINDS
NEW CLINICAL
RESEARCH PROTOCOLS:
![]()
The following new protocols were approved in March:
- A Pilot Study of Treatment of Adults with Sickle Cell Disease Associated Pulmonary Hypertension Based on Hemodynamic Stratification: Safety and Tolerability Study of Imatinib and Carvedilol; 12-H-0093; Dr. Gregory J. Kato; NHLBI
- Novel Imaging Modalities to Characterize Angiogenesis in the Bone Marrow Microenvironment in Multiple Myeloma (MM) and its Precursor Disease; 12-C-0106; Dr. Carl O. Landgren; NCI
- Carfilzomib, Lenalidomide, and Dexamethasone in High-Risk Smoldering Multiple Myeloma: A Clinical and Correlative Study; 12-C-0107; Dr. Carl O. Landgren; NCI
- Validating a New Writer's Cramp Scale; 12-N-0104; Dr. Mark Hallett; NINDs
- Phase I/II Study of Metastatic Cancer Using Lymphodepleting Conditioning Followed by Infusion of Anti-mesothelin Gene Engineered Lymphocytes; 12-C-0111; Dr. Steven A. Rosenberg; NCI
- Bisphenol A (BPA) Pharmacokinetic (PK): Controlled Exposure Study; 12-E-0089; Dr. Stavros Garantziotis; NCI
- A Phase 1 Study of Imetelstat, a Telomerase Inhibitor, in Children with Refractory or Recurrent Solid Tumors and Lymphomas; 12-C-0091; Dr. Brigitte C. Widemann; NCI
- Clinical and Molecular Manifestations of Neuromuscular and Neurogenetic Disorders of Childhood; 12-N-0095; Dr. Carsten G. Bonnemann; NINDs
- Collection of Granulocytes by Apheresis of Healthy Donors Stimulated with Filgrastim (G-CSF) and Dexamethasone; 12-CC-0096; Dr. Susan F. Leitman; CC
- Energy Expenditure Responses to a Range of Environmental Temperatures around the Thermal Neutral Zone; 12-DK-0097; Dr. Kong Y. Chen; NIDDK
- Pharmacogenetics and Neuroimaging in Major Depressive Disorder (PAN-D); 12-M-0099; Dr. Gonzalo Laje; NIMH
- Oral Microbial and Immunological Characterization of Patients with Immune Dysfunction; 12-D-0100; Dr. Niki M. Moutsopoulos; NIDCR
- Measurement of the Reactive Hyperemia Index in Sickle Cell Patients During Pain Crisis and After Recovery; 12-H-0101; Dr. Hans C. Ackerman; NHLBI
- Characterization of Innate Immune Responses to MF59 Adjuvanted H5N1 Vaccine Compared to Non-adjuvanted H5N1 Vaccine; 12-H-0103; Dr. Shira Y. Perl; NHLBI
QUICK LINKS:
![]()


Stop searching on your own for clinical studies.
Let opportunities to join a study find you.
The NIH Clinical Center has joined ResearchMatch, an online, national clinical research registry that "matches" people who want to participate in clinical studies with researchers who are seeking volunteers. To learn more, visit researchmatch.org/?rm=Volunteer3
Clinical Center Nutrition Department feeds young minds at science festival
 |
| CC Executive Chef Robert Hedetniemi's cooking demonstration showcased MyPlate, a tool from the US Department of Agriculture that helps people understand the major food groups and proper portions. |
When most people think of hospital food, they don't picture fine dining. And when some individuals think of healthy eating, they don't imagine a delicious dinner and dessert.
So the NIH Clinical Center's Nutrition Department worked on changing perceptions at the second annual US Science & Engineering Festival in Washington, DC April 28-29 with a cooking demonstration that showcased the science of simple, healthy cooking and tasty tips the audience could incorporate into their daily routines.
The CC's Executive Chef Robert Hedetniemi prepared a culinary spread consisting of pistachio-encrusted salmon, Mediterranean-style quinoa, wilted rainbow Swiss chard with caramelized onions, and a key lime parfait. The meal was planned around the US Department of Agriculture's MyPlate, an icon designed to help people learn healthy eating habits consistent with the 2010 Dietary Guidelines for Americans. MyPlate replaced the traditional food pyramid in 2011.
 |
| The CC Nutrition Department emphasized that cooking fresh can be healthy and tasty at their demonstration at the US Science & Engineering Festival on April 28 in Washington, DC. |
Jennifer Widger, a CC Nutrition Department manager and registered dietitian, accompanied Hedetniemi during the presentation to emphasize the educational concepts. "MyPlate is taking the five basic food groups—the dairy, protein, grains, fruits and vegetables—and making sure that you try to get a little bit of that on every plate and in every meal," explained Widger.
Nutrition Department team members are experts at not only healthful eating but also restaurant-quality preparation. They prepare and deliver food, customized to their nutritional needs, to all of the inpatients and day hospital patients throughout the CC. The hospital's unique Room Service Program also allows patients to place orders anytime between 6:30 am to 6:30 pm and receive their order with 45 minutes.
David Folio, chief of the Nutrition Department, explained that the point of the demonstration was to help people understand the science of healthy eating and "show that you can eat this way, in a simple way, with foods from your grocery store."
Hedetniemi simmered and sautéed in front of the crowd, which seemed to grow as the smell of food wafted through the DC convention center. Although Hedetniemi put on a good show, Folio added, "You don't have to be an executive chef to do this."
Hedetniemi agreed and said it is all about eating healthy and having fun. "I would say jump in with both feet. Get something in your pantry. That's the first step. The battleground is in the supermarket," he said. "Bring the stuff home and when you have it in your pantry, you might be more inclined to actually take the step to one day and actually experiment. And if you make a mistake, it's a bump on the road to success."
For more information on the CC Nutrition Department's exhibit at the US Science & Engineering Festival, including recipes and the MyPlate meal example, visit clinicalcenter.nih.gov/scienceexpo/index.html.
Researchers find method to improve transplant cell delivery
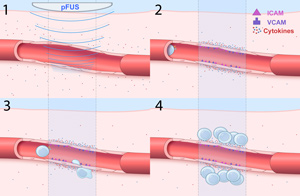 |
| NIH researchers discovered that pulsed focused ultrasound elevates levels of naturally produced chemicals on target tissues. Transplanted stem cells have receptors for these chemicals, so an increased presence attracts more of them to the desired site. |
A new technique for improving delivery of stem cells may lead to better and faster tissue repair, a breakthrough with promise for sports medicine and military populations.
Clinical Center researchers discovered a way to enhance delivery of transplant cells in rodents to a desired site by increasing presence of chemicals that attract the introduced cells. Non-destructive pulsed focused ultrasound interacts with tissue to elevate levels of naturally produced chemicals (such as cytokines, chemokines, and growth factors) on target tissues. Transplanted stem cells have receptors for these chemicals, so an increased presence attracts more of them to the desired site.
Regenerative medicine uses stem cells to replace damaged cells and tissues, and transplanting these cells intravenously is a noninvasive and easily replicated procedure. However, only 1 to 3 percent of intravenous transplanted cells make it to the desired target. By increasing the presence of chemically attractive factors, researchers in the laboratory saw 8 to 10 times more transplanted bone marrow stromal cells in a pulsed focused ultrasound-treated rodent kidney than a non-treated kidney.
"It's like your circulatory system is a series of highways. What makes you want to get off at New York City? We're putting an attraction in the middle of nowhere so the transplant cells will want to go there, to the target site," said Dr. Joseph A. Frank, chief of the CC Radiology and Imaging Sciences Laboratory of Diagnostic Radiology Research. Frank is senior author on the findings which were published online in Stem Cells on March 30.
The attractive chemical agents are enhanced during inflammation or injury, but their quantity elevations last for a short time. Researchers in the laboratory showed that they can extend that window or open a new one using pulsed focused ultrasound. The ultrasound delivers energy to a targeted region, and the tissue converts the energy into the chemical attractive agents. The ultrasound increased the number of these agents expressed on endothelial or vessel wall surfaces through approximately one day and returned to control levels by day three.
An advantage of this improved delivery method is that the pulsed focused ultrasound does not cause any adverse effects to the treated tissue. Researchers also saw increased passage of stem cells into treated tissue and retention, and the focused ultrasound permeates deep so human body composition is not a limitation. Since the technique increases presence of more than 10 attractive chemical factors, the method is not cell specific and may be advantageous for a variety of cell products, such as neural cells or immune cells.
"This research shows the ingenuity of our scientists and the fostering environment at the NIH Clinical Center to run with an idea and see it through to real application for clinical practice," said Dr. John I. Gallin, CC director.
Researchers from the National Cancer Institute; Catholic University of America, Washington, DC; and the National Institute of Biomedical Imaging and Bioengineering also contributed to these findings.
Longtime Clinical Center advocate Susan Butler honored
 |
| Clinical Center Director Dr. John I. Gallin (left) presented Jim Butler with a plaque honoring the memory of his wife, Susan Lowell Butler, a passionate advocate for CC patients. |
The Clinical Center honored longtime friend Susan Lowell Butler on April 30 with a dedication ceremony and unveiling of a plaque installed on the seventh floor atrium honoring her memory and contributions as a patient and an advocate. Butler died on December 18, 2010.
"Susan was a determined, articulate advocate for patients who participate in clinical research, and in that she left a long-lasting imprint on the Clinical Center," said CC Director Dr. John I. Gallin at the unveiling.
An active member of the CC community since she sought treatment here for simultaneous diagnosis of breast and ovarian cancer in 1995, Butler was an original member of the Patient Advisory Group and the consumer representative on the NIH Advisory Board for Clinical Research. She was a keynote speaker at the dedication ceremonies for the new Mark O. Hatfield Clinical Research Center in 2004 and was selected to be the patient greeter of President Barack Obama during his 2009 NIH visit. She also served as a faculty lecturer for the CC course "Introduction to the Principles and Practice of Clinical Research" and contributed the only patient-written chapter to the course's textbook.
An enthusiastic and involved advocate for cancer patients, Butler co-founded the Ovarian Cancer National Alliance. She was founder and past chair of the Ovarian & Gynecologic Cancer Coalition/Rhonda's Club, and the executive director of the DC Cancer Consortium.
"This is such a great honor for Susan," Butler's husband Jim said. "She was a fierce advocate and wasn't afraid to voice her opinion about things, but she combined that with a sense of mirth and good humor."
Department of Transfusion Medicine staff member mourned
 |
| Lavora Dash, a phlebotomist in the CC Department of Transfusion Medicine, died in April. |
Lavora Clark Dash, a phlebotomist in the Clinical Center Department of Transfusion Medicine (DTM) for eight years, died unexpectedly on April 21.
"Her commitment to the Department of Transfusion Medicine was powerful, and her spirit and humor often raised the spirits of those around her," said Dr. Susan Leitman, DTM Blood Services Section chief, recalling the hundreds of donors who requested her when they came to donate and Dash's reputation as one of the best phlebotomists in the department. "This is a great loss for all of us, and it is hard to really comprehend that she is gone."
Tracey Chinn, acting chief nurse of the DTM Blood Services Section, and Bonnie Sink, Blood Services Section clinic manager and Dash's direct supervisor, remember her as a positive, cheerful, and encouraging member of their team. "She worked well with first-time donors and donors who were nervous. She would talk to them and make them feel better," said Sink.
Chinn said that Dash was known for her cheerful sayings, thanking people for coming to work at the end of the day and announcing that, "Sunshine is here, hold the applause," when she herself arrived. "She really had a larger-than-life spirit, and her sayings and attitude created such a positive environment," said Chinn.
Dash was a devoted sister and a loving mother. She leaves behind two teenage children, ages 18 and 14.
Mannes named Department of Perioperative Medicine chief
 |
| Dr. Andrew Mannes was named chief of the Clinical Center Department of Perioperative Medicine in April. |
Dr. Andrew Mannes was named chief of the Clinical Center Department of Perioperative Medicine (DPM) in April.
Before the appointment, Mannes was a staff clinician in the DPM, where he worked with the CC Pain and Palliative Care Service and laboratories of the National Institute of Dental and Craniofacial Research pain and neurosensory mechanisms branch in the area of pain management.
He has a long-standing interest in the treatment of severe pain often seen at the end-of-life. Current research includes developing pain therapies using gene therapy; targeting pain pathways with selective agonists, toxins or fusion proteins; and improving the diagnosis of disease states with the use of proteomics and genomics techniques.
Mannes' goal as chief is to expand DPM's educational programs to include more opportunities for training and research fellowships. "There aren't many anesthesiologist clinician-scientists in the United States, and that is a need that has been recognized," he said. "This is a wonderful opportunity to develop academic research programs and to train investigators to excel in translational science."
Mannes received a bachelor of science degree in bio-engineering from the University of Pennsylvania and a master of engineering from Dartmouth College. He completed his medical training at The George Washington University and a transitional internship at the Presbyterian Hospital of Philadelphia, followed by a residency in anesthesiology at the Hospital of the University of Pennsylvania. There he completed a fellowship in pain management and joined the Penn faculty as an instructor in anesthesiology and was promoted to assistant professor of anesthesiology before coming to the NIH. Mannes has been in the Department of Anesthesia and Surgical Services (now DPM) since 2001.
"Under Dr. Mannes' leadership, I am confident that the Department of Perioperative Medicine will develop into a superb academic anesthesiology program and that the department will continue to provide outstanding clinical research support service to NIH investigators and patients," said Dr. John I. Gallin, CC director.
Practice makes perfect—Staff tests emergency preparedness skills
 |
| Ann Peterson, Clinical Center clinical nurse specialist, practices using the hospital's electronic medical records system. |
A team of Clinical Center experts in white lab coats huddle around their patient and shout questions.
"Do we know if this patient is on any medications?"
"Could we see if it's in their record or ask the patient?"
"OK, does anyone know this patient's primary language?"
As the patient triage unfolds in the research hospital's patient transport entrance, it can be easy to forget that this patient—and all of the other patients in the disaster preparedness drill on April 26—exist only on paper.
"We chose to use paper patients so we could focus on the tools. Often, when we have actual patients, we spend so much time focusing on them because they are looking back at us," said Mary Sparks, a nurse consultant for the CC deputy director for clinical care. "Today's training is about getting more familiar with technology that we use during emergencies but may not use in our daily practice." Sparks explained that these tools include hand held radios, video telephones, and software program for electric medical records. "Technology is supposed to help us work more efficiently," added Sparks, "but the only way that can happen is with practice."
The drills are an annual occurrence as part of the Bethesda Hospitals Emergency Preparedness Partnership between Walter Reed National Military Medical Center, the NIH CC, Suburban Hospital, and the National Library of Medicine. The partnership was formalized in 2004. Through these exercises, the organizations get the chance to cross-train, teambuild, and strengthen collaborative readiness in the National Capital Area.
A key part of this readiness is leveraging resources, explained Sparks. In fact, the partnership was recently recognized with an HHSinnovates award for a technology the team developed to electronically track transfer patients during disasters. The technology will be used by the partnership facilities, but is also an exportable model that can be deployed and tailored to work in other medical settings.
Editor's note: Read more about the HHSinnovates award.
Patient tracking and locating system wins HHSinnovates award
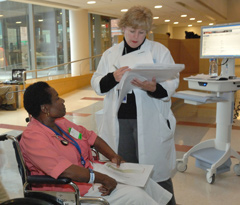 |
| The award-winning system is tested during the annual Bethesda Hospitals' Emergency Preparedness Partnership disaster drill pictured above. |
The Clinical Center, the National Library of Medicine, and their partners in the Bethesda Hospitals' Emergency Preparedness Partnership (BHEPP) won a coveted HHSinnovates award for developing a suite of tools to help hospitals manage the surge of patients during a disaster.
The portable, electronic system provides real-time information on the number of incoming patients, the severity of their injuries, and their location within the hospital so key personnel can quickly make strategic decisions about patient care and safely share information when patients are moved from one hospital to another.
"This award is evidence of the NIH commitment to collaborative innovation that will have broad application for the betterment of patient care and human health," said CC Director Dr. John I. Gallin.
US Health and Human Services Secretary Kathleen Sebelius named the Patient Tracking and Locating System as a "Secretary's Pick" in the latest HHSinnovates awards announced March 30. The system was conceived and developed by the NLM. It was tested during disaster drills by the public-private BHEPP: the CC, the NLM, and the Walter Reed National Military Medical Center, and Suburban Hospital Johns Hopkins Medicine.
"The Clinical Center and our BHEPP colleagues truly are honored to receive this award. One of the central goals when the partnership was formed some six years ago was to develop an exportable model for managing patient care during disaster situations," said Laura Lee, special assistant to the CC deputy director for clinical care and CC BHEPP lead. "I know that the partnership team is thrilled that our collective efforts have resulted in an innovation that can be deployed throughout the broader health care community – both in the United States and globally."
The BHEPP's mission is to develop a coordinated response to disasters that could serve as a model for hospitals in communities across the country. The Patient Tracking and Locating System is one of several disaster management tools developed and studied as part of the BHEPP.
The NLM's Patient Tracking and Location System includes:
- a digital pen that captures patient information on paper and electronically
- software that allows data from the pen and tracking system to be collected, stored, and shared electronically
- an application to securely transfer parts of a patient's record from one hospital to another
- a real-time location system that uses infrared and radio-frequency to track the locations of patients from the time they arrive at a hospital until the time they leave the facility
The awards ceremony can be viewed at youtube.com/user/USGOVHHS [disclaimer].
Patient safety interventions at CC reduce risk, improve care
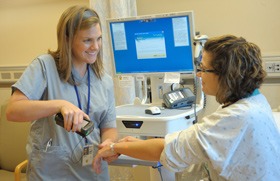 |
| Barcode technology is one patient safety intervention CC staff use to verify patient identity. |
The Clinical Center is committed to ensuring that all patients experience safe and high quality care and has implemented strategies in three key areas to improve patient safety throughout America's research hospital, including:
Preventing patient falls
Patient injuries due to falls are a significant safety issue at any health-care facility, said Laura Lee, special assistant to the deputy director for clinical care. The CC has a Falls Prevention Program designed to reduce the risk of harm to CC patients from falls of any kind. Each patient is assessed for potential risk for falling. If a patient is determined to be at high risk, special precautions are implemented to reduce the chance of an incident, including placing a "falling star" sign on the patient's door and chart to alert staff that the patient is at risk for falling, and assuring that the patient only walks with assistance. Other strategies include moving the patient closer to the nursing station and using bed alarms to alert staff if the patient tries to get out of bed without assistance. Lee says that these strategies have reduced the CC's rate of falls to a much lower rate compared to other hospitals in the United States.
Medication reconciliation
Medication reconciliation is how the health-care team makes sure that a patient receives the appropriate medications while in the hospital. At the CC, this process begins at admission, when the care team works with the patient to collect accurate information about the medications that the patient has been taking at home. A critical step in the reconciliation process is a careful review by a CC pharmacist who compares the list of medications that the patient provides with the medications ordered by the care team. Any discrepancies are "reconciled" through a discussion with the practitioner who prescribed the medications. This double-check assures that patients get the correct medications when they are admitted.
Barcode technology
Verifying the identity of patients prior to collecting specimens, transfusing blood and blood products, or administering medications is crucial to patient safety. CC staff identity patients by first asking them for their names and dates of birth. The CC also invested in bar-coding technology as a means to verify patient identity and to match orders to the individual patient. Barcoding has been implemented for specimen collection and transfusion verification in the last two years and will soon be implemented for medication administration.
DLM staff saluted during lab week
 National Medical Laboratory Professionals Week honors the more than 280,000 medical laboratory professionals across the nation who perform and interpret laboratory tests that assist with patient care. Pathologists, senior staff, laboratory technologists, phlebotomists, and technicians at the Clinical Center are among the many heroes of health care who aid in the diagnosis and treatment of patients across the country. The Department of Laboratory Medicine performs about 1.5 million laboratory tests each year and provides critical support to CC and NIH staff. The department also supports active fellowships in chemistry, hematology, and microbiology and maintains vigorous research programs in each of the department's services.
National Medical Laboratory Professionals Week honors the more than 280,000 medical laboratory professionals across the nation who perform and interpret laboratory tests that assist with patient care. Pathologists, senior staff, laboratory technologists, phlebotomists, and technicians at the Clinical Center are among the many heroes of health care who aid in the diagnosis and treatment of patients across the country. The Department of Laboratory Medicine performs about 1.5 million laboratory tests each year and provides critical support to CC and NIH staff. The department also supports active fellowships in chemistry, hematology, and microbiology and maintains vigorous research programs in each of the department's services.
The department honored laboratory professionals for their contributions through staff appreciation events planned by the Lab Week committee pictured above. For more information on the DLM, visit clinicalcenter.nih.gov/cp/index.html.
Medical Record Department celebrates health information professionals week

The Clinical Center Medical Record Department celebrated Health Information Professionals Week March 25 – 31, recognizing the department's staff members and leadership for their commitment to delivering quality health care through quality information.
The MRD celebrated with a gathering recognizing the team for their role in ensuring that health information for all CC patients contains the most accurate data possible and that the information is used correctly. Pictured above are several staff members who joined in on the celebration including (from left) David Richey, Shannon Matthews, Tricia Coffey, Ron DeClerck, David Rice, and Tonica Johnson.
CC hosts annual pharmacology meeting
 |
| Robert DeChristoforo, CC Pharmacy Department chief, gave meeting attendees a virtual tour of the Pharmaceutical Development Section. |
The Clinical Center hosted the 21st annual Association of Clinical Pharmacology Units (ACPU) meeting in April.
The meeting offered a critical forum for the exchange of information and ideas among investigative sites involved in early phase clinical research.
Presentations focused on the future of clinical pharmacology units and models for emergency response coverage for first-in-human studies. Dr. Juan Lertora, director of the CC clinical pharmacology program, and Dr. John McKew, chief of the National Center for Advancing Translational Sciences therapeutics development branch, presented "Drug Rescue and Repurposing Initiatives at NIH."
Pharmacy Department Chief Robert DeChristoforo gave a virtual tour of the CC Pharmaceutical Development Section with a focus on the facility's features in compliance with the US Food and Drug Administration's current good manufacturing practices.
Participants also heard from Dr. Clare Hastings, CC chief nursing officer, on the evolving role of nurses in early phase clinical research.
Said Dr. Fatemeh Tavakkoli, a recent graduate of the University of Maryland School of Pharmacy, "The access to patients, scientists, and resources offered here is magnificent."
Office of Workforce Management and Development quick tip: staying motivated
Staying motivated during complex times, that was the focus of the Clinical Center Office of Workforce Management and Development Leadership Development Brown Bag series in March.
The session offered perspectives from a panel of CC supervisors including Denise Ford, Office of Hospitality Services chief; Brenda Robles, Language Interpreters Program coordinator; and Anita Segar, 5SW nurse manager. They offered three key ideas for staying motivated and keeping those around you motivated during complex times:
1. "Feeling gratitude without expressing it is like wrapping a present without giving it." In order for people to be connected and motivated, they need to feel valued. It is critical for leaders to acknowledge everyone's contributions to the work environment.
2. "Amidst the worst situation, there is beauty. You can flourish despite the harsh ground." Leaders should share the bigger picture and help their team see the goal.
3. "Make time for face time." Knowing your team helps with your credibility. Learn what motivates them. Understand their unique needs. This helps create the conditions for motivation and opens a space where differences are respected and common ground can be found.
The next Leadership Development Brown Bag series is "Got Change? Manage Your Expectations." It's set for May 30 in the Hatfield Medical Board Room (4-2551).
Clinical Center news briefs
Pharmacy staff member recognized
Daniel Zlott, a clinical pharmacy specialist in the CC Pharmacy Department, received the Hematology/Oncology Pharmacy Association (HOPA) New Practitioner Award at the 2012 HOPA annual meeting in Orlando. The award cites Zlott for being, "a clinician, teacher, researcher, and leader who has affected positive patient outcomes and has the potential to significantly improve oncology pharmacy practice."
NIH Back-Up Care Program
The NIH has contracted with Bright Horizons® to offer employees back-up care when they need to be at work and their regular child or adult/elder care is unavailable. NIH employees must verify eligibility before registering and the registration process must be completed before they can use the care. Requests for care can be placed one month in advance and up to the day care is needed. For more information, visit backupcare.ors.nih.gov.
Race for a cure with Team NIH
Join Team NIH for the Susan G. Komen Global Race for the Cure—a 5K (3.1 mile) walk or run to support breast cancer research on the National Mall in Washington, DC, on June 2. There is a $40 registration fee, but no additional fundraising is required.
Choose "Join a Team" and search for Team NIH at globalrace.info-komen.org [disclaimer]. Organizers will send an email with details on where and when to meet before the race. Contact Maggie McGuire at mcguirema@mail.nih.gov for more information.
Research Participant Education Committee resources
Did you know the Research Participant Education Committee has a growing website of patient education resources for CC staff? Included are links to the latest infection control guidelines, CC-specific patient information, and blood and marrow transplant resources. Visit the RPEC website to learn more at, intranet.cc.nih.gov/rpec/index.html (NIH staff only).
 Celebrate Hand Hygiene Day
Celebrate Hand Hygiene Day
Staff, patients, and visitors are invited to I ♥ Clean Hands Day in the Clinical Center atrium on May 23, from 11 am - 2 pm. Enjoy fun activities that emphasize the importance of proper hand hygiene and vote for your favorite hand washing promotional poster.
Protect your patients, your family, and yourself. Learn when and how to sanitize at intranet.cc.nih.gov/hospitalepidemiology/hand_hygiene.shtml (NIH staff only).
Try a little PLC (Plain Language Care)
Guide your reader
Headings inform readers like guideposts along a street. Readers use headings to help them find information efficiently.
Write Headings with heft
Headings beginning with "How to" may delay your reader's understanding. Readers tend to notice the words "How to" so that all headings seem the same. Look at this example:
- How to get a work order
- How to fill out a work order
When headings start with action verbs, readers easily find what they want, as in this example:
- Getting a work order
- Filling out a work order
Keep heading forms consistent
If you start using headings with questions, try to use that format throughout the document.
Effective headings show that your writing has Plain language care. If you have questions about using plain language in your writing, refer to clinicalcenter.nih.gov/plain.html or email Wendy Schubert at wschubert@nih.gov.
NOTE: PDF documents require the free Adobe Reader.
 The information on this page is archived and provided for reference purposes only.
The information on this page is archived and provided for reference purposes only.