Patient move date shifts as activation continues
The date for patients to move into the Mark O. Hatfield Clinical Research Center has changed. "Our target is January 8, 2005," said Dr. John I. Gallin, Clinical Center director.
"I made this decision to allow adequate time for further testing and validation of the new facility's major systems. Simply put, we have to make sure that new hospital and the equipment in it works as expected. We'll spend the next weeks testing and validating that it does."
Many moves and changes in preparation for full activation will continue on schedule.
As of Dec. 5:
- The main entrance for the Clinical Center will shift of the lobby of the Hatfield Center, which is on the north side of the complex on Center Drive.
- Patient shuttle stops will move to the main entrance of the Hatfield Clinical Research Center. There will no longer be patient shuttle service from the south entrance of the Magnuson Center.
- Who parks where in the Clinical Center garages changes; see sidebar below for specifics.
As of Dec. 6:
- Valet parking for patients and visitors will relocate to the main entrance of the Hatfield Center.
- Campus and campus express shuttles will stop at both the Hatfield and existing Magnuson Center stops. All off-campus shuttles will continue to use the south entry.
By early December, most of the laboratory moves will be complete and core patient services will have relocated to the new hospital, including Admissions, the Cashier and Voucher offices, and Patient Travel on the first floor and Social Work on the second. However, no patients will be cared for in the building until the patient move. Hospitality desks will be open at the main entrance and in the lobby adjacent to P1 parking for patients.
"The new hospital is a large and complex building," Gallin added. "We are committed to the highest standards of patient care. I appreciate your tireless work in supporting the activation of this remarkable new hospital, and look forward to this next exciting stage.
Back
to Top
Garage parking shifts December 5
Parking in the Clinical Center's underground garages will shift as of Dec. 5.
- The P1 level, which is off Convent Drive, will be for patients and their visitors. Handicapped parking will also move to P1. Individuals who park in P1 have direct access to the CRC's lower-level lobby.
- The P2 level will be for patient-care staff and staff with red permits. Drive through the P1 entrance on Convent Drive and proceed to the P2 level.
- The P3 level, which is off Memorial Drive, will provide general employee and reserved-space parking.
Parking attendants will be stationed on all levels to assist motorists.
Back
to Top
Emergency drill jump-starts new partnership

A firefighter and a mass-casualty evaluator assist a victim simulating injuries during the mass-casualty exercise at the National Naval Medical Center. Photo by Photographer's Mate Airman Adam Herrada, U.S. Navy (RELEASED).
|
On October 21, nearly simultaneous explosions rocked Bethesda. A radiological bomb had detonated at the National Naval Medical Center (NNMC),
followed almost instantly by explosions at a nearby Metro station. Mass casualties were reported and traffic along Rockville Pike, which separates NIH from NNMC, came to a standstill.
That was the scenario of a drill that tested and evaluated a new emergency preparedness partnership that includes the Clinical Center, Suburban Hospital and NNMC. As part of the exercise, some participants portraying seriously injured patients, replete with makeup of mock injuries, were transferred from NNMC, through the NIH campus, to Suburban Hospital, which lies to the immediate west of NIH across Old Georgetown Road. So that Suburban could accept the influx of "patients" from NNMC, participants portraying stable patients were transferred from Suburban to the Clinical Center.

Ginnie Daine, Nursing, and Dr. Fred Gill, chief, Internal Medicine Consult Service, assist in admitting patients at the Clinical Center.
|
It was the first time the Clinical Center, NNMC and Suburban Hospital conducted a joint drill. They recently formed a new emergency preparedness partnership to strengthen the regional response to disasters in the metropolitan area. A major goal of the exercise was to demonstrate how the three hospitals would work together to provide an effective regional response.
A fleet of fire emergency vehicles from Montgomery County; NIH; Naval Surface Warfare Center, Carderock; Walter Reed Army Medical Center, Naval District Washington; and NNMC took part, as obstacles such as simulated car accidents were cleared and emergency vehicles navigated the necessary routes of access.
Preceding the exercise, more than 40 distinguished guests from the U.S. Department of State, Department of Health and Human Services, Department of Homeland Security and other local, state and federal emergency management agencies attended a press conference to kick off the event.
"It's always a privilege to work closely with neighbors," said Dr. John I. Gallin, director of the Clinical Center. "Today's exercise jump-starts a historic partnership and alliance that brings together…the complementary expertise and resources of the National Naval Medical Center, Suburban Hospital and the NIH Clinical Center."
On behalf of Navy Rear Adm. Adam Robinson, commander, NNMC, Capt. Mark Olesen, deputy commander, welcomed Rep. Chris Van Hollen, of Maryland's Eighth Congressional District; Doug Duncan, Montgomery County executive; Gallin; and Brian Gragnolati, CEO of Suburban Hospital. Oleson also praised the effort, saying it would put the new partnership to the test. "In less than an hour," he said, "we will get to test and evaluate our partnership, maximizing the strengths of our extensive decontamination capacity with the clinical resource base and sophisticated ...facilities of the National Institutes of Health and the…Trauma Center and acute care of Suburban Hospital."
Other participants included representatives from the Office of Attending Physician at the U.S. Capitol, District of Columbia Hospital Association, Bureau of Medicine, Public Health Service, Department of Veterans Affairs, Bethesda/Chevy Chase Rescue Squad, Montgomery County Health Department Emergency Planning Committee and the Montgomery Country Fire Rescue Service.
Gallin said the partnership "exceeds what can be accomplished individually. Coordinated collaboration is essential to an effective regional response to an emergency."
The partnership, he added, was created to foster this collaboration-and to demonstrate how two government agencies and a private-sector institution can work together for the betterment of all.
Gallin praised the CRC's new capabilities, which will add state-of-the art space for hospital care and the Clinical Center's nursing and health care staff, which he called "second to none and always up to a challenge."
- by John Iler
Back
to Top
From MIS to CRIS:
A look back at changing technologies
CRIS's recent go-live was a tremendous challenge, but nothing like the one the Clinical Center faced in 1976, when it introduced its first electronic information system. The system CRIS replaces was a pioneering effort in its day: a large-scale electronic medical information system (hence MIS) to keep track of previously handwritten medical orders and patient-care data. Some hospitals had begun using computers to keep track of billing, but with MIS the Clinical Center converted manual operations and information handling to a computerized hospital information system that reflected its priorities: clinical research and patient care. It was ahead of its time.
It was not warmly welcomed.
MIS went live for inpatient documentation one nursing unit at a time, starting with neurology, a unit in which physician's orders flowed heavily. Anxiety was nearly universal. Nurses, who played a natural role overseeing the flow of patient-centered information and requisitions, took the lead in training multidisciplinary teams in the new technology.
One of their tasks was to quell resistance from doctors. Retired nurse Alice Duncan remembers one doctor in neurology saying, "I am not going to use this computer. This is for a bank! This is not for a medical professional!"
For the older doctors, especially, MIS's introduction was traumatic. Young doctors today grow up with e-mail, spreadsheets, and data entry, but in 1976 one nurse saw a surgeon hit the computer, he was so frustrated with its refusal to take his order. The head of cardiac surgery went up to his nursing unit at two o'clock in the morning, unplugged the equipment, and took it off the ward.
Vernice Ferguson, chief nurse at the time, insisted that nurses not transcribe physician orders-that physicians must enter their own orders, to avoid introducing another level of errors. Considering that other hospitals weren't even implementing such clinical systems, the level of compliance with Ferguson's insistence on physician-entered orders was astonishing. Dr. Mort Lipsett, the physician-scientist who became Clinical Center director after MIS was designed and ordered, pushed the system through despite resistance. As soon as everyone got used to it, they began griping about its limitations, but nobody ever suggested going back to handwritten orders.
The forward-thinking MIS team (led by Drs. Tom Lewis, Roderick Prior and David Swedlow, all physicians, and industrial engineer Jerry Macks) adapted the system to make it more palatable to doctors and more responsive to the needs of research protocols. The core system handled charting, clinical orders, and retrieval of results for all NIH inpatient and outpatient visits. It was expanded by accretion, with the addition of ancillary systems (to exchange information with the pharmacy, diagnostic radiology, laboratory testing, the blood bank, and so on).
MIS was ahead of its time and, with continual customization, did a good job for 28 years. But the expectations the vendor software generated were quickly disappointed and as research studies and clinical care became more complex, the old technology couldn't meet the Clinical Center's changing needs. Instead of one terminal per nursing unit there was a computer on every desk and laptops for work at home or on trips. The world had gotten hooked on computer technology and expected far more from it.
By its nature, MIS was never built to support research, says Dr. Steve Rosenfeld, Clinical Center's chief information officer. "It was a hospital information system, not a research system, and that's all it was." The MIS team's goal had been to support the research process by automating data retrieval. MIS could collect patient data but support for research protocols was limited by the vendor technology, a proprietary database, and a fairly inflexible closed system.
In 2002, the Clinical Center accepted bids for development of a clinical research information system to replace MIS. Rosenfeld led the development team and Dr. Cliff Lane, a senior investigator with NIAID, headed the steering committee.
"A hospital information system is essentially a tool kit for building a model of how your hospital should operate," says Rosenfeld. "These systems don't come with a starter set. You have to design almost everything from scratch, from where orders go and what orders look like to how things are used."
The team that developed CRIS included technical people (working on hardware, software, and networks), physicians and nurses with clinical training and informatics backgrounds, and staff working on interfaces (connecting clinical data). The Eclipsys Corporation (which also provided MIS's core software) developed the core patient-care system. Wherever possible, CRIS systems were designed around commercial off-the-shelf (COTS) products marketed for clinical care.
A group of 150 users from different departments spent time logging real patient data and testing everything they could, documenting problems ("I can enter pills but not injections") and asking questions. Their questions and those that came up in training became 400 frequently asked questions for a user's manual. A slim pocket user's guide was also printed.
CRIS represents the next generation of medical information technology. Two dozen distinct information systems will plug into two broad CRIS hubs: a clinical data repository (for patient care) and a clinical data warehouse (for research).
The repository will include the electronic medical record, housing information about patient care and hospital operations-such things as a patient's lab results, pharmacy orders, doctors' and nurses' notes and other documentation. In the second phase, which will take at least another six months (including the move to the new hospital), CRIS will take over registration and scheduling, the two functions MIS still handles. To complete the upgrade, other CRIS capabilities will be activated, including rules ("for every patient on this protocol, don't allow this drug to be ordered"); alerts and reminders (which will help resolve many problems with pharmacy); pathways (sets of orders that can be laid out over days on the calendar, immensely useful for protocols); and flow sheets.
 |
The CRIS team is looking at adding a separate pharmacy system; a surgical system (scheduling, materials management, documentation for surgery and anesthesia); systems for critical care and radiology; and links to patient's diagnostic images (through a Web-based viewer for images, under development in Diagnostic Radiology). MIS was text-based and so far CRIS is too, but as it develops CRIS will be able to display diagnostic and other images.
The new system will eventually add protocol mapping, a new tool for authoring, documenting, and managing research protocols. Think of a protocol map as a matrix, with certain requirements along the left axis—such as medications, treatments, diet, education requirements—and along the horizontal axis Day One, Day Two, Day Three, and so on. Protocol mapping will allow a protocol to become a set of care plans for a patient and will also generate data for the research database.
The clinical data warehouse will collect longitudinal patient data for use in research (while protecting patient privacy and confidentiality). The two systems will be separate so that demand on the research system won't slow down the fast delivery of information on the patient-care system.
This is part two in a two-part series.
- by Pat McNees
Back
to Top
In Memoriam
Barbara Beall, 35, a social worker for the Social Work Department, passed away at home in August after a year's bout with cancer. But just days before, she was where she wanted to be—at work.
"I want to die with my boots on," she told coworkers.
She had just celebrated her birthday on July 24. Many of her closest friends were those with whom she worked.
"She was so very skilled in her ability to relate to all kinds of people throughout her career," said Dr. Adrienne Farrar, head of the Social Work Department and Beall's supervisor, at an October 15 memorial service eulogy. "She took pride in coming to work—of being available and accessible in doing her job," which she did until July 29, her last day of work. "She left us smiling and with a plan to come back the next day with a list of things that she would do upon her return."
After completing her student placement in the NIH Social Work Department, Beall became a social worker in 1993, working first for NIAID and later for NCI in pediatric oncology. She was to begin work at the NIH Family Lodge in 2005. She was diagnosed with breast cancer in July 2003.
"She was a consummate professional with a passion for her patients, their families and the research mission of our institution," said Dr. Lauren V. Wood, senior clinical investigator, HIV & AIDS Malignancy Branch, NCI. "She was a valiant soldier in her battle against cancer and a living witness of what it means to fight the good fight. Her star will continue to shine…in the hearts of those who knew and loved her."
According to her coworkers, Beall had an outgoing personality. "She was bubbly and warm," said one. "She liked things that sparkled, regardless of their value, and she loved costume jewelry." In a dedicatory song at the memorial service written to the tune of "My Favorite Things" and written by Beall's friend and colleague Tina Levin, her friends sang:
"Jewelry and sparkle, hairdos and hair colors;
parties and road trips, the beach was her druthers.
Loved to read books, could do crosswords all day;
lotions and perfumes, they all were her way."
"She also brought in the most delicious treats," another coworker said.
The song continues:
"Generous, kind and courageous and gutsy,
she was the contract supplier from Eatzi's;
she never told us that she bought the food,
sandwiches, cookies—it was all so good."
"Barbara had one of the most irreverent, razor sharp and wicked senses of humor of anyone I ever met," Farrar said, "…and we loved her for saying what so many of us wanted to say in observing life and all of its ironies and complexities."
The song:
"Chocolate and Pepsis and swirled margaritas,
swore like a sailor, ate Guapos' fajitas;
beautiful inside and beautiful out,
this is our Barbara; we miss her no doubt."
Beall is survived by her parents; her brother, Patrick; and her sister, Diana.
Back
to Top
Emanuel becomes latest Clinical Center
physician to be elected to the IOM

Dr. Ezekiel Emanuel.
|
On October 18, Dr. Ezekiel Emanuel, Department of Clinical Bioethics, became the latest Clinical Center physician to be elected to the prestigious Institute of Medicine (IOM), joining Dr. Harvey Alter and Dr. John Gallin in this honor. Emanuel was elected to the Institute in recognition of his work in bioethics. The IOM issues reports providing information and advice about health and science policy to Congress, other policymakers and the general public.
New members of the IOM must be sponsored by a current member and are elected by the current membership. Election is based on professional achievement in a field related to medicine and health; involvement with issues of health care, disease prevention, education, or research; and skills that will contribute to the Institute's work of assessing current knowledge, conducting studies, and considering policy issues.
"It's a great tribute to be elected to the IOM," said Emanuel, "It represents recognition by your peers that you are making important contributions to the biomedical field."
With his election, Emanuel was honored for his achievements in bioethics, from helping to improve end-of-life care to his work in research ethics and health policy. "One of the main purposes of the IOM is to offer objective and independent advice to the government, so it frequently is asked by Congress and other government and nongovernmental organizations to investigate issues," said Emanuel. "The Institute often investigates bioethical issues, and I hope to be actively participating in panels related to these issues."
A breast cancer specialist, Emanuel was appointed chair of the Clinical Center's Department of Clinical Bioethics in 1998. He received his MD from Harvard Medical School and his PhD in political philosophy from Harvard University. His doctoral dissertation received the Toppan Award for the finest dissertation in political science of the year. Emanuel was a fellow in the program in ethics and the professions at the Kennedy School of Government and Harvard. After completing an internship and residency in internal medicine at Boston's Beth Israel Hospital and an oncology fellowship at the Dana-Farber Cancer Institute, Emanuel joined the faculty at the Dana-Farber Cancer Institute. He was also associate professor at Harvard Medical School. Emanuel served on the ethics section of President Clinton's health care task force and on the National Bioethics Advisory Commission. He has published widely in medical journals on the ethics of clinical research, advance care directives, end-of-life care issues, euthanasia, the ethics of managed care, and the physician-patient relationship. His book on medical ethics, The Ends of Human Life, received honorable mention for the Rosenhaupt Memorial Book Award by the Woodrow Wilson Foundation. He received the AMA-Burroughs Wellcome Leadership Award and a Fulbright scholarship (which he declined).
One of four components of the National Academies of Science, the IOM was established in 1970 to serve as adviser to the nation to improve health. Recent reports issued by the Institute include advice on preventing childhood obesity, the ethical conduct of clinical research involving children, the safety of genetically engineered foods, biological threats and terrorism, and improving palliative care for cancer patients.
Back
to Top
NIH-Duke Training Program
in Clinical Research
Applications are being accepted for the 2005–2006 NIH-Duke Training Program in Clinical Research.
Implemented in 1998, the program is designed primarily for physicians and dentists who want formal training in the quantitative and methodological principles of clinical research. Courses are offered at the NIH Clinical Center via videoconference technology. Academic credit earned by participating in this program may be applied toward satisfying the degree requirement for a Master of Health Sciences in Clinical Research from Duke University School of Medicine. The degree requires 24 credits of graded course work, plus a research project for which 12 units of credit are given. The program is designed for part-time study, allowing students to integrate the program's academic training with their clinical training.
Applications are available in the office of Clinical Research Training and Medical Education, Building 10, Room B1L403. Information about coursework and tuition costs is available on the program website at http://tpcr.mc.duke.edu.
Enrollment in this program is limited. If you are interested, inquire with your Institute/Center about funding for participation. E-mail queries about the program may be addressed to tpcr@mc.duke.edu. The deadline for applying is March 1, 2005. Successful applicants will be notified by July 1, 2005.
Back
to Top
Massage therapy available to Clinical Center patients
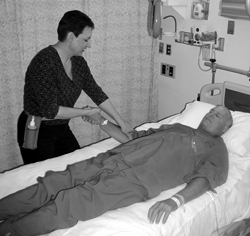
Hartman says many of her requests come from savvy patients who know, or have heard, that the massage therapy program exists.
|
Joanie Hartman got into massage therapy the easy way. She experienced it for herself. She was so "touched," one might say, that she decided she wanted to learn it. And her training and dedication to it brought her to the recreational therapy section of the Clinical Center's Rehabilitation Medicine Department.
"I suppose it's like anything else," Hartman said. "You learn a lot by receiving massages, and then by practicing it. To get a license, one has to attend school, take courses and study the body's bone and muscle structure. Since I had the interest, I decided to just do it."
She did and soon enrolled at the Potomac Massage Training Institute. There she learned about various techniques of therapeutic massage and the importance of touch in healing. And though there are many forms of massage, from Swedish to deep tissue, Hartman's specialty is shiatsu, which works on acupressure points. Most types are pleasant and instantly relaxing to patients; others, like deep tissue and an aggressive deep muscular manipulation known as "Rolfing," can initially be grueling, but provide substantial relief of bodily and emotional tension.
Requests for patient massages come from a nurse or nurse practitioner. "At least 60 percent of my referrals come through Dr. Ann Berger, chief of the Pain and Palliative Care Service," Hartman said. "And some come from patients, especially those with back pain." In some cases, she added, one patient will tell another who is unaware of the therapy and word gets around. "But some patients don't know that I'm here, so they don't know how to ask for it, so it's a balance."
Massage therapy has received some tremendous feedback and Hartman would like others to know that massage therapy is available. Benefits include reduction of pain and anxiety and reduction of stress. "One patient had a headache for eight days and requested massage to get rid of it," Hartman said. "And it did. Sometimes just touching people makes them feel better."
But massage therapy, which is often accompanied by soothing music with a slow rhythm, also has long-lasting effects, especially for patients who are bedridden. The manipulation of the muscles forces toxins such as lactic acid, which cause soreness and restlessness, out into the bloodstream where they can be flushed from the human body.
"Another patient said his experience was as if he were floating on a river and he thought it was remarkable."
Hartman is available to patients all day Monday and Friday and on Wednesday evenings. She can be reached at 301-496-8876.
- by John Iler
Back
to Top
CRC conference room
reservations
Conference rooms in the CRC will become available for meetings and other events on December 6. Of the 39 conference rooms, nine are centrally scheduled, 12 are scheduled by Clinical Center departments, and 18 are scheduled by various clinical offices.
Six of the centrally scheduled conference rooms are managed by Clinical Center hospitality services. Located on the third and fifth floors of the CRC, they hold 22 to 30 people. To schedule these six rooms, e-mail a request to hatfieldconferencerooms@cc.nih.gov.
Three larger rooms, holding 45 to 65 people, are managed by the NIH Events Management. Located on the second and fourth floors of the CRC, they can be scheduled by calling Building 10 Conference Room Services, 301-496-9966 (select option 4), or by submitting a request at: www.nih.gov/od/ors/dirs/mapb/websch.htm.
The departmental conference rooms, located in or near the Clinical Center departments, hold 12 to 40 people. All rooms are furnished and are equipped with pull-down video screens and audio conferencing capabilities. Rooms that hold more than 20 people also have video projection, an audio system, VCR and DVD, and computer connections. Each Clinical Center department determines its own scheduling procedures for its conference room. Contact the department directly for more information.
Clinical area conference rooms are located in or near patient care areas and each area determines its own scheduling procedures. Room capacity ranges from 15 to 37. All rooms are furnished and equipped with a pull-down screen and audio conference capability. Contact the clinical area directly for more information.
Back
to Top
Flu shots canceled: Those at risk are exceptions
Even as the ink was drying on the October issue of CCNews—including the table outlining when flu vaccines would be available to Clinical Center employees—national media sources reported a vaccine shortage because of the contamination of vaccines produced by Chiron Corporation, in England.
All healthcare workers with direct patient care responsibilities and patients who meet the CDC priority list immunization should receive a flu shot. Staff who do not provide direct patient care are asked to forgo or defer vaccination unless they fall into the priority list for immunization.
Pregnant healthcare workers are encouraged to receive the vaccine, particularly if they are in their second or third trimester during respiratory virus season. The vaccine is safe for both mother and infant if the mother is breast-feeding.
Those most at risk during the flu season include all children aged 6 to 23 months; adults 65 and older; those aged 2 to 64 who have underlying chronic medical conditions; women who will be pregnant during the influenza season; residents of nursing homes and long-term care facilities; children aged 6 months to 18 years on chronic aspirin therapy; and out-of-home caregivers and household contacts of children under 6 months old.
People cannot catch the flu from the injectable vaccine—it is a killed viral vaccine that has no live organisms in it."
For more information about fly vaccine availability at the Clinical Center, call the Occupational Medicine Service, 301-496-2209.
Back
to Top

|


