From the Clinical Center to a disaster zone
Public Health Service professionals help after hurricanes hit in 2017
Interested in helping when a future crisis strikes? Members of the U.S. Public Health Service can sign up for a Rapid Deployment Force with their supervisor's approval.
Other federal employees can enroll in the Surge Capacity Force, which is maintained by the Department of Homeland Security and supports the Federal Emergency Management Agency's (FEMA) urgent response and recovery efforts. Learn more.
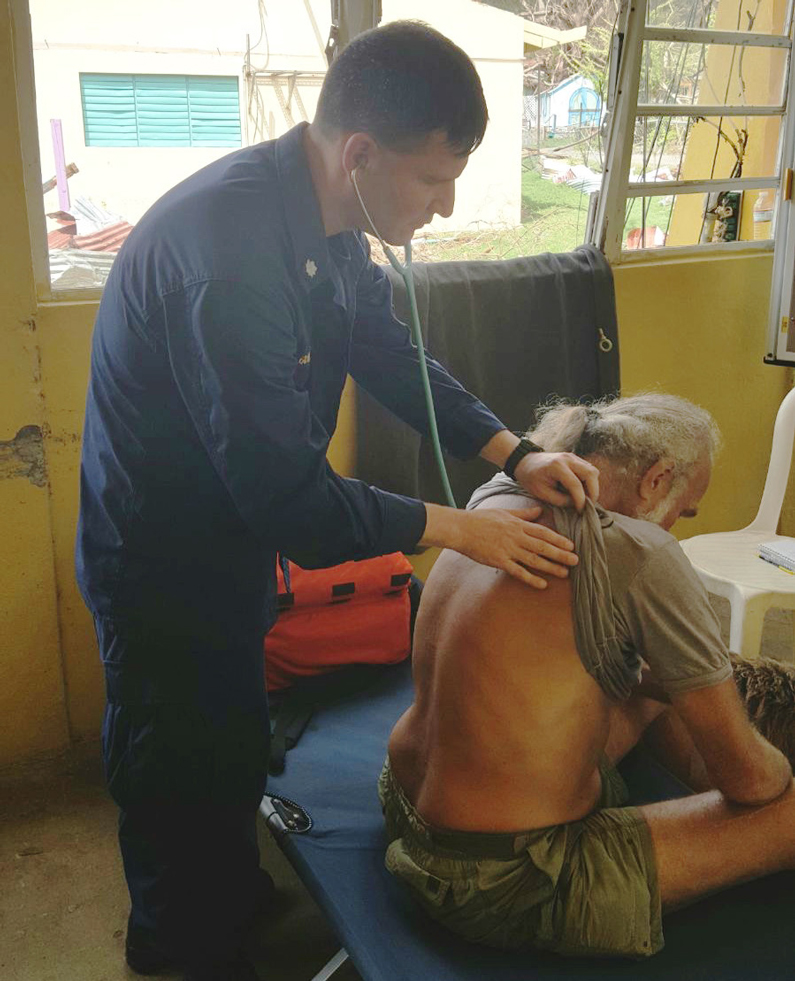



When a life-threatening storm is bearing down, most people wouldn't think of the NIH Clinical Center. But employees who work in the hospital were among the many responders helping Americans devastated by hurricanes in 2017.
The National Oceanic and Atmospheric Administration predicted that 2017 would be an active hurricane season, and storms hit many parts of the continental United States and Caribbean territories with Hurricane Harvey landing in Houston, Hurricane Irma hitting Florida and the Caribbean, followed by Hurricane Maria whose destructive power left Puerto Rico without power.
Soon after the first storm made landfall, officers of the U.S. Public Health Service who work in the Clinical Center were activated to provide support. Overseen by the Surgeon General, the U.S. Public Health Service Commissioned Corps is a diverse team of more than 6,500 public health professionals. They fill essential public health leadership and clinical service roles with the nation's federal government agencies, including the NIH.
Daniel Goldstein, a physician assistant and commander in the U.S. Public Health Service, works in the Clinical Center for the National Heart Lung and Blood Institute (NHLBI). Goldstein has seen the impact of extreme weather events before, having been deployed to help in the recovery of New Orleans after Hurricane Katrina hit in 2005.
This time he was assigned to a new mission in the U.S. Virgin Islands. He travelled through all three of the islands that make up the territory, but spent most of his time between the east and west parts of St. John, supporting an urgent care center and providing medical care at temporary shelters. The treatment he provided was critical as the area's hospital was destroyed.
The Virgin Islands had planned ahead, flying out their most critically ill patients before the storms hit, so relief efforts focused on urgent care medical services, particularly treatment of fractures, infections, and medication refills.
Adapting to the situation required that we "be flexible to the mission and expect the unexpected," said Goldstein.
Despite their hardships, he said the residents of the Virgin Islands have a "close community" and it was great to see "people looking out for each other" even in such a time of turmoil.
Cmdr. Ulgen Fideli, also a U.S. Public Health Service physician assistant with NHLBI in the Clinical Center, was deployed to Florida to help people who had kidney failure, and required dialysis treatment.
Fideli knew a lot about kidney disease as her father had received dialysis treatment for years before passing away earlier this year. When Fideli saw the news coverage of the hurricanes, she said "I knew I had to do something."
Fideli traveled to Atlanta and from there he was deployed to Miami. The patients she saw weren't from Florida, however. They were evacuees from the U.S. Virgin Islands.
These were full care patients, a sick population who had chronic diseases and mobility issues, said Fideli. Not only did they have health issues, but they had gone through multiple displacements from their homes to temporary spaces in Puerto Rico and finally to a shelter in Miami. Along the way many lost their bags and medications. According to Fideli, the travel and uncertainty was "taking a toll."
Despite the challenges, there were some uplifting moments. "We would see the same people every day and developed a sense of camaraderie," she said. The security guards at the shelter introduced the staff to Cuban coffee, served in tiny but potent cups.
The day after Fideli's deployment ended, she received word that the residents of the shelter had been moved again, this time to Federal Emergency Management Agency housing in Atlanta.
Seeing so many vulnerable people going through so much hardship was really "humbling," reflected Fideli. "It puts everything in perspective when you come back."
Lt. Melanie Webb, a nurse who works in the NIH Clinical Center's Office of Patient Recruitment, was deployed to Ponce in the southern part of Puerto Rico about two hours from the capital of San Juan. Flying to Ponce, Webb saw the extent of the island's destruction out of the plane's window.
Webb worked in an 80-bed field medical station based in a repurposed basketball stadium, the most stable building in the community, despite its leaky roof.
The patients they served would typically have received home care but they were displaced because of the storm. Due to the overwhelming damage to the community, the care Webb and others provided often extended not just to the patient but to their whole family.
On a regular basis, Webb and her colleagues would conduct "strike missions" where they would travel by military vehicles to bring medical assistance to communities isolated by the damage. They helped treat minor wounds, replenish supplies of medications and, when needed, transported people in medical crisis back to the field hospital.
For Webb, the destruction of homes and infrastructure was truly stunning.
"Usually we treat patients and send them back to the community," said Webb. "But there was no community to send them back to."
-Donovan Kuehn

